[Product Collection] 03 Simulation Model – Peripheral Interventional Vascular Model | High-Precision 3D Data for Accurate, Empowering Simulations
Release date:
2025-08-28 15:20
Peripheral vascular disease affects a large and growing number of people. From 2021 to 2030, the volume of peripheral artery intervention procedures in China is projected to surge from approximately 163,000 cases to about 602,000 cases, representing a compound annual growth rate of 15.6%. Meanwhile, the number of peripheral vein intervention procedures is expected to climb dramatically—from roughly 201,000 to 1.529 million, reflecting an impressive CAGR of 25.3%. The market for peripheral artery intervention stents and balloons is also anticipated to experience significant growth during this period. From 2021 to 2030, the market size for these devices is forecasted to expand from RMB 2.17 billion to RMB 6.73 billion, with a compound annual growth rate of 13.4%.
Preface
Peripheral vascular disease affects a large and growing number of people. From 2021 to 2030, the volume of peripheral arterial intervention procedures in China is projected to surge from approximately 163,000 cases to about 602,000 cases, representing a compound annual growth rate of 15.6%. Meanwhile, the number of peripheral venous intervention procedures is expected to climb dramatically—from roughly 201,000 cases to 1.529 million cases—driven by a robust compound annual growth rate of 25.3%. The market for peripheral arterial intervention stents and balloons is also anticipated to experience significant expansion. From 2021 to 2030, the market size for these devices is forecasted to grow from RMB 2.17 billion to RMB 6.73 billion, reflecting a steady compound annual growth rate of 13.4%.
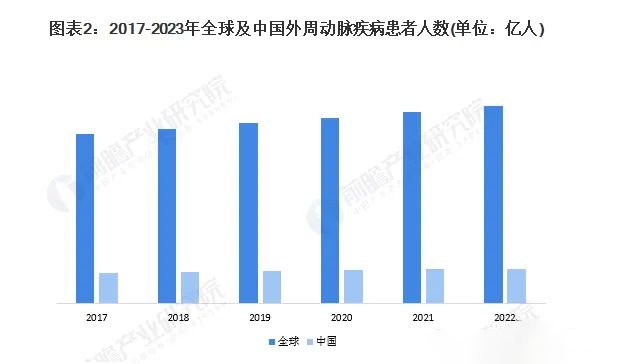
▲ Image reprinted from: Qianzhan Research Institute
Surgical technique development
In the early 20th century, Dawbam pioneered the concept of interventional therapy by using embolization with a plug to occlude the external carotid artery. Vascular imaging techniques emerged in 1923, and in 1929, Fotsmann first introduced cardiac catheterization for angiography. Then, in 1953, Seldinger developed the percutaneous femoral artery puncture technique for angiography, laying the foundation for modern interventional procedures.
In 1964, Dotter performed the first percutaneous transluminal angioplasty, marking the transition of interventional procedures from diagnosis to treatment. Subsequently, techniques such as arterial catheter-directed hemostasis and embolization for gastrointestinal bleeding emerged one after another. During the 1970s and 1980s, advancements in intravascular devices like stents and balloons significantly enhanced both the efficacy and safety of interventional therapies.
Starting in the 1990s, peripheral intervention entered a mature phase. New embolic materials and advanced catheters and guidewires emerged, enabling more precise treatments. Meanwhile, treatment applications expanded beyond vascular diseases to include tumors and non-vascular luminal conditions. The integration of medical imaging with interventional techniques has further enhanced visualization and safety. In recent years, peripheral intervention has begun to combine with gene and cell therapies, while the growth of telemedicine is also bringing benefits to an increasing number of patients. Looking ahead, breakthroughs in this field are expected to extend into even more diverse areas.
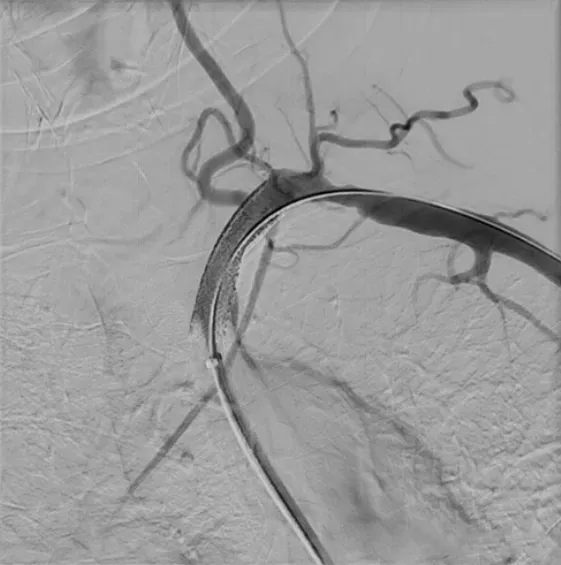
▲ Peripheral Interventional CT Image (Image source: Internet)
Model Structure
●Thoracic aorta + Abdominal aorta + Peripheral vessels (hepatic artery + renal artery + splenic artery + superior mesenteric artery) + Lower limb arteries (iliac artery, femoral artery, popliteal artery, anterior tibial artery, posterior tibial artery, peroneal artery) + Bilateral upper limb arteries (subclavian artery + axillary artery + brachial artery + radial artery)
● Superior vena cava + right heart + pulmonary artery + inferior vena cava + renal veins + lower limb veins (iliac vein, femoral vein, popliteal vein, anterior tibial vein, posterior tibial vein, peroneal vein) + bilateral upper limb veins (subclavian vein + axillary vein + brachial vein + radial vein)

▲ Overview of the DeWei Medical Peripheral Interventional Vascular Model
Model Features
I. Surgical Training and Education
1. Simulate a real-world operational environment
Replicating the anatomical structures of peripheral vessels—such as the femoral, popliteal, and carotid arteries, as well as veins—includes features like vessel diameter, curvature, branch angles, and pathological conditions (e.g., stenosis, aneurysms, thrombosis). These models are designed to help doctors practice skills such as puncture techniques, guidewire and catheter manipulation, and stent placement.
For example: By simulating femoral artery stenosis, doctors can be trained to refine their precision in balloon angioplasty or stent placement.
2. A Practice Platform with Controllable Risks
Avoid the risks of real surgery while enabling repeated practice until proficiency is achieved—perfect for novice doctors to master interventional procedures and manage complications, such as vascular perforation or dissection.
It can be combined with imaging equipment (such as a DSA simulator) to train intraoperative image-guided navigation and path-planning skills.
II. Interventional Device Development and Testing
1. Performance Verification
Testing the pushability, compliance, and wall-apposition properties of novel devices such as guidewires, catheters, stents, and balloons in simulated blood vessels.
For example: Evaluating the expansion performance and drug-release uniformity of drug-coated balloons in simulated narrowed blood vessels.
2. Optimize design parameters
By analyzing how the device performs in different vascular morphologies—such as tortuous vessels or bifurcation lesions—based on model feedback, we can guide design improvements and enhance its clinical applicability.
Supporting domestic medical device R&D: Accelerating the localization of peripheral intervention devices—such as domestically produced stents and thrombectomy devices—to reduce reliance on imported products.

▲ Detailed view of Derui Medical's peripheral vascular intervention model
3. Medical Research and Pathology Simulation
1. Disease Model Construction
Simulating various peripheral vascular disease scenarios, such as arteriosclerosis obliterans, deep vein thrombosis, varicose veins, and vascular malformations, to study disease mechanisms and develop effective treatment strategies.
Example: In a simulated deep vein thrombosis model, test the thrombolysis efficiency of a novel thrombolytic catheter.
2. Hemodynamic Studies
Using computational fluid dynamics simulations, we analyze how different interventional procedures—such as stent placement—affect blood flow velocity and pressure distribution within blood vessels, while also predicting post-procedure outcomes and identifying potential risks, like in-stent restenosis.
Combine computer simulations—such as finite element analysis—to optimize surgical plans and device designs.
4. Teaching and Science Communication Exhibits
1. Visual Teaching Tools
Designed for medical students or patient education, these transparent or 3D-printed models visually demonstrate vascular structures, lesion patterns, and the principles of interventional procedures, helping to clarify complex medical concepts.
2. Surgical Simulation and Treatment Planning
For complex cases—such as long-segment occlusions or bifurcation lesions—preoperative modeling is used to simulate the surgical approach and develop a personalized treatment plan, thereby reducing intraoperative uncertainty.
5. Quality Control and Standardization
Providing a standardized testing platform for interventional device manufacturing, ensuring products meet clinical use requirements (such as dimensional accuracy and mechanical performance).
Assist in establishing industry standards to promote the standardization and homogenization of peripheral intervention techniques.

|

|
Application
The peripheral vascular intervention model is widely used in the medical field. During surgical training, it simulates real-life vascular anatomy and pathologies—such as stenosis and thrombosis—allowing doctors to repeatedly practice procedures like puncture and stent placement. This helps reduce risks in actual surgeries and is particularly beneficial for beginners to master the procedural workflow.
During device development, it’s possible to test the pushability and wall-apposition properties of devices such as guidewires and stents, optimize design parameters, and accelerate innovation in domestically produced medical devices.
In medical research, it is possible to establish disease models such as atherosclerosis and deep vein thrombosis, and combine these models with hemodynamic analysis to assess how interventional procedures affect blood vessels, thereby aiding in the exploration of underlying pathological mechanisms.
Additionally, the model can also be used for visualized medical education of students, preoperative simulations for complex cases, and standardized quality control in device manufacturing, thereby promoting the standardized development of interventional techniques.
Keywords:
Other news
Request a quote
*Please keep your phone accessible—we'll reach out to you within 24 hours.









