[Product Collection] 03 Simulation Model – Hepatic and Renal Artery Interventional Vascular Model | Pulse Pathway Simulation, Precision in Intervention
Release date:
2025-08-22 12:42
Hepatic and renal artery intervention originated in the mid-20th century. In 1953, Seldinger's invention of percutaneous vascular puncture—featuring a minimally invasive technique that uses a guidewire to guide catheters—laid the foundation for interventional therapies, inspiring doctors to explore the application of vascular access in treating liver and kidney diseases.
[Product Collection] 03 Simulation Model – Hepatic and Renal Artery Interventional Vascular Model | Pulse Pathway Simulation, Precision in Intervention
I. History of the Procedure
Hepatic and renal artery intervention originated in the mid-20th century. In 1953, Seldinger's invention of percutaneous vascular puncture—featuring a minimally invasive technique that uses a guidewire to guide catheters—laid the foundation for interventional therapies, inspiring doctors to explore the application of vascular access in treating liver and kidney diseases.
In the 1970s, angiography technology matured, providing clear visualization of the hepatic and renal arterial structures and offering precise "navigation" for interventional treatments. In 1974, Japanese researchers introduced transcatheter arterial embolization (TAE) as a treatment for liver cancer, effectively blocking the tumor's blood supply by occluding its feeding arteries, thereby significantly prolonging survival in patients with advanced-stage liver cancer—a major breakthrough in hepatic intervention therapy. Around the same time, the field of renal artery interventions also saw remarkable progress: in 1978, balloon angioplasty was first applied to treat renal artery stenosis, restoring adequate blood flow to the kidneys by expanding the narrowed segments, thus addressing the clinical challenge of renovascular hypertension.
Since then, techniques such as stent implantation and selective arterial chemoembolization have emerged one after another, transforming hepatic and renal artery intervention from a single treatment modality into a comprehensive system encompassing diagnosis, therapy, and monitoring—and ultimately revolutionizing the approach to treating liver and kidney diseases.
The instruments required for the procedure include guidewires, catheters, embolic materials, stents, and more. However, hepatic and renal vascular structures are highly complex and exhibit significant individual variability. For instance, the liver may present with variations in the hepatic artery or disordered tumor vasculature, while the kidneys often face challenges such as tiny and intricately angled renal artery branches. In complex cases, it’s difficult to fully assess the suitability of existing devices and their therapeutic efficacy before surgery—for example, when dealing with multi-arterially supplied liver cancer lesions, it’s hard to determine the optimal dosage and distribution of embolic materials. Moreover, the surgical techniques involved are exceptionally demanding; even a slight mistake could lead to serious complications like damage to normal liver or kidney function, or unintended ectopic embolization. To address these challenges, interventional vascular models of the hepatic and renal arteries have been developed.
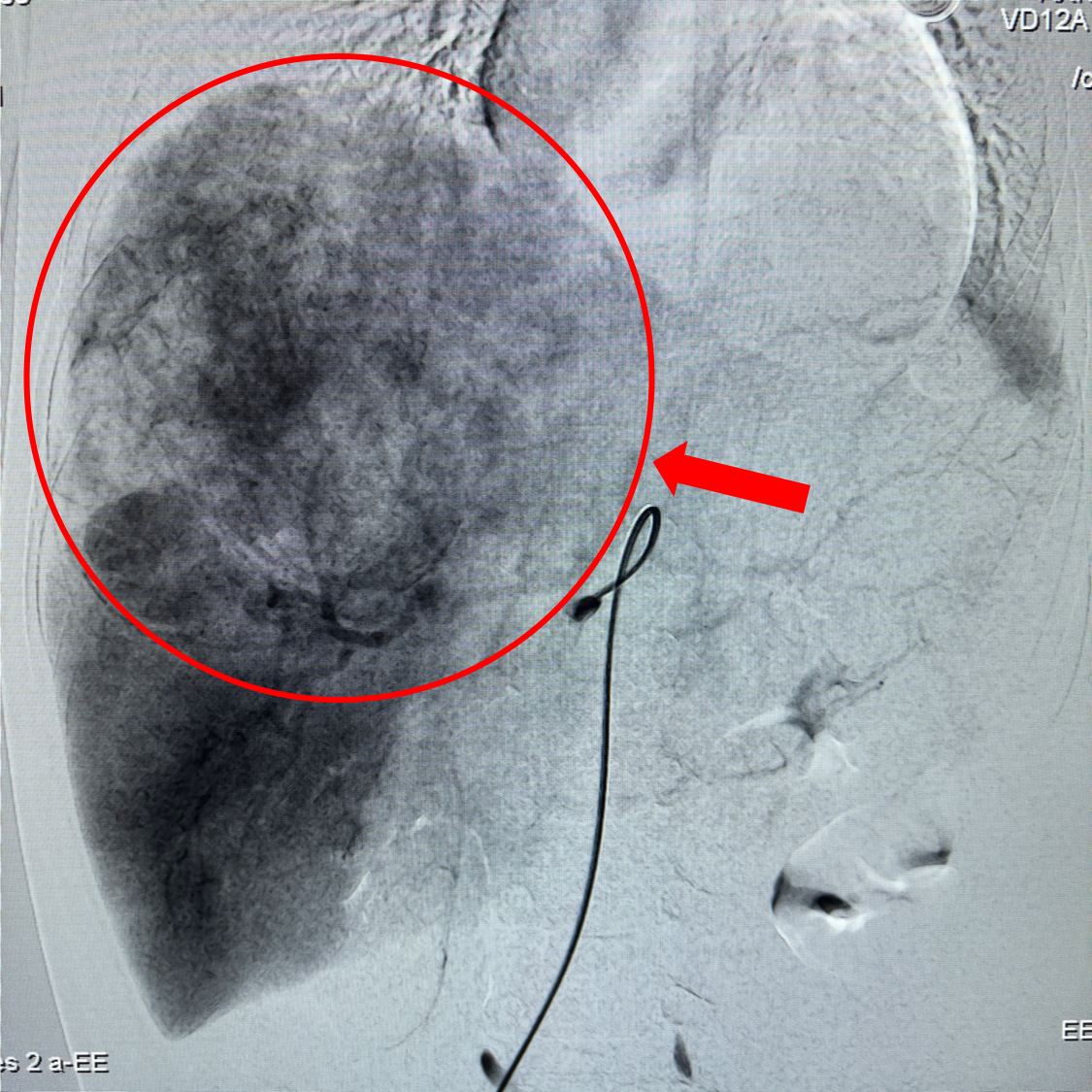
CT image of a hepatic artery tumor (Image source: Internet)
II. Structure
Abdominal aorta + complete hepatic artery + splenic artery + renal arteries ++ iliac artery (2 cm above the iliac bifurcation)
The liver and kidney arterial interventional vascular model is crafted using a self-developed, medical-grade high-polymer silicone material, combined with high-precision 3D printing technology to precisely replicate the anatomical structures of the liver, kidneys, and their associated arteries. Within the model, branches of the hepatic artery—such as the proper hepatic artery, left hepatic artery, and right hepatic artery—are rendered with lifelike accuracy, even simulating common vascular variations. Meanwhile, the multi-level branching pattern of the renal artery as it originates from the abdominal aorta, along with its precise relationship to the renal segments, is accurately depicted. The vessel walls exhibit authentic elasticity and resilience, allowing them to mimic how blood vessels change shape in response to varying blood flow pressures.
The model is equipped with interchangeable lesion modules that can simulate various pathological conditions, including liver cancer nodules, hepatic hemangiomas, renal artery plaques, and kidney tumors. Moreover, the vascular morphology and hemodynamic changes at the lesion sites are accurately replicated. In addition, the model supports connection to a circulatory system simulator, allowing users to adjust parameters such as blood flow velocity and pressure to mimic both normal and pathological blood flow scenarios. Furthermore, the model seamlessly integrates with digital subtraction angiography (DSA) equipment, delivering lifelike angiographic images during operation and providing users with an immersive surgical simulation experience.

Overview Diagram of the Hepatic and Renal Artery Intervention Model – Xi'an Derui Medical
3. Functions and Applications
Function:
The hepatic and renal arterial interventional vascular model plays a multifaceted and critical role in medical practice. In the fields of medical education and skills training, it precisely replicates the branching structure of the hepatic and renal arteries, the characteristics of the vessel walls, and common lesion patterns—such as stenosis, malformations, and tumor-induced angiogenesis—enabling medical students and young physicians to repeatedly practice procedures like puncture, catheter superselection, and embolic agent injection. This hands-on experience helps them become proficient with interventional workflows and equipment, allowing them to quickly develop both technical dexterity and valuable clinical expertise.
When faced with complex clinical cases, this model can be personalized using patients' CT and MRI imaging data, accurately simulating real vascular anatomy and pathological conditions. This provides surgeons with a preoperative planning platform, allowing them to rehearse surgical procedures on the model, test the feasibility of various interventional approaches and device combinations, anticipate potential risks during surgery—such as vessel rupture or ectopic embolism—and develop tailored strategies to mitigate these risks, ultimately enhancing the safety and success of the actual procedure.
In scientific research and device development, the model simulates various physiological and pathological conditions, providing a testing platform for the development of innovative embolic materials, drug-eluting stents, and more. This helps researchers validate technical feasibility and accelerates the translation of groundbreaking innovations into clinical applications.
Applications:
In the field of medical education, the liver and kidney artery interventional vascular model serves as a core tool for nurturing specialized professionals. Medical schools use this model to deliver hands-on interventional procedures courses, enabling students to progressively master complex techniques such as superselective arterial catheterization—starting from basic skills like vascular puncture and guidewire placement. The model can simulate a variety of pathological conditions, including hepatic artery stenosis and renal artery anomalies, helping trainees gain valuable experience in managing intricate clinical cases and effectively shortening the transition period from theoretical learning to real-world practice. Additionally, the standardized nature of the model facilitates teaching assessments, allowing instructors to promptly identify and correct any improper techniques based on students' performance during simulations.
In clinical practice, this model has become a "virtual rehearsal sandbox" that helps doctors develop surgical plans. For patients requiring interventional treatments—such as those with liver or kidney cancer—doctors can use the patient’s CT and MRI data to create personalized models. These models allow surgeons to simulate embolization pathways beforehand, test stent deployment outcomes, and anticipate potential intraoperative risks like vascular spasm or embolic agent reflux. By doing so, the surgical strategy can be refined, ultimately boosting the success rate of treatment. Additionally, some hospitals are using these models to visually demonstrate the procedure to patients and their families, improving communication between doctors and patients while helping to ease patient anxiety.
At the intersection of scientific research and industrial innovation, the model serves as a testing platform for developing new interventional devices. Researchers can simulate various hemodynamic environments to evaluate the performance of innovative embolization microspheres and drug-eluting stents. Meanwhile, companies can leverage the model to validate the maneuverability of catheters and guidewires, accelerating product iteration and upgrades while driving the ongoing advancement of hepatic and renal arterial intervention techniques.
This model supports simulations of various procedures, such as hepatic arterial chemoembolization, hepatic hemangioma embolization, renal artery stenting, and renal tumor arterial embolization. Through repeated simulation practice, physicians can enhance their procedural skills and precision, providing more reliable technical support for interventional treatments of liver and kidney diseases—and ultimately advancing medical progress in these critical fields.
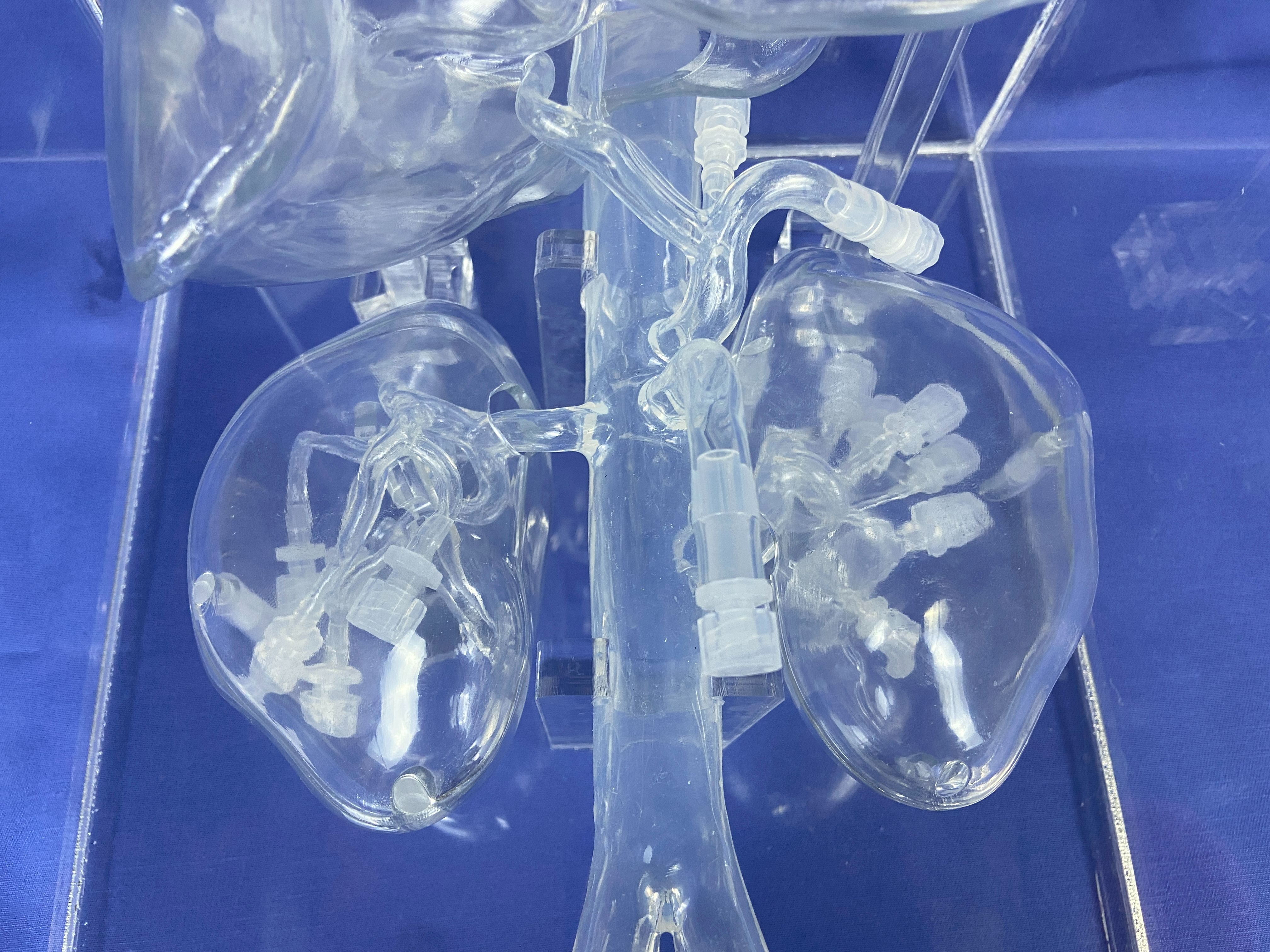
Close-up of the interventional model details for hepatic and renal arteries — Xi'an Derway Medical
Keywords:
Other news
Request a quote
*Please keep your phone accessible—we'll reach out to you within 24 hours.









