[Product Collection] 03 Simulation Model – Pulmonary Artery Intervention Vascular Model | Modular Components
Release date:
2025-09-05 09:47
The evolution of pulmonary artery intervention therapy reflects the continuous exploration and breakthroughs in the medical field. In the 1980s, pioneering physicians first began experimenting with balloon angioplasty to address pulmonary artery stenosis, marking the dawn of interventional treatment for this condition. Since then, catheter-guided techniques have steadily gained prominence, offering unparalleled precision in targeting lesions while enhancing both the accuracy and safety of procedures. As a result, these advancements have significantly improved treatment outcomes and patient safety, firmly establishing interventional therapy as the mainstream approach for managing pulmonary artery stenosis today.
One . Surgical technique development
The evolution of pulmonary artery intervention therapy reflects the ongoing exploration and breakthroughs in the medical field. In the last century, 80 In those years, medical pioneers began experimenting with balloon dilation techniques to address pulmonary artery stenosis, marking the dawn of interventional therapy for pulmonary arteries. Since then, catheter-guided technology has steadily gained momentum, offering unparalleled precision in targeting treatment areas. This advancement has made procedures not only more accurate and safer but also significantly improved both therapeutic outcomes and patient safety—solidifying interventional therapy as the leading treatment approach for pulmonary artery stenosis over time.
Diseases such as pulmonary embolism, pulmonary artery stenosis, and pulmonary arteriovenous malformations pose serious threats to patients' lives and health. Pulmonary embolism requires rapid removal of the clot blocking blood vessels via catheter-based thrombolysis or thrombus aspiration, restoring proper lung circulation. Patients with pulmonary artery stenosis rely on balloon angioplasty or stent placement to widen the narrowed vessels. Meanwhile, those with pulmonary arteriovenous malformations typically undergo treatment involving coil embolization or the use of embolic agents to block abnormal blood vessels.
This procedure relies on instruments such as guiding catheters, microcatheters, guidewires, thrombus aspiration devices, balloon dilation catheters, and embolic coils. However, the pulmonary arterial system features intricate branching, thin vessel walls, and highly variable clot morphologies—ranging from long, floating thrombi to wall-adherent clots—making it exceptionally prone to vascular rupture or perforation during manipulation. Moreover, pulmonary vessels are closely situated near the heart and bronchial arteries; even minor deviations in instrument handling during the procedure could lead to life-threatening complications like massive hemorrhage or air embolism. On top of this, some patients have compromised cardiopulmonary function, making them unable to tolerate prolonged surgical interventions. As a result, surgeons must demonstrate both exceptional precision and remarkable speed in their techniques. Traditional training methods, however, fall short in replicating the real-world pathological conditions and the associated complex risks. This is precisely why the development of pulmonary artery intervention models has emerged as a critical breakthrough, helping surgeons overcome longstanding technical challenges.
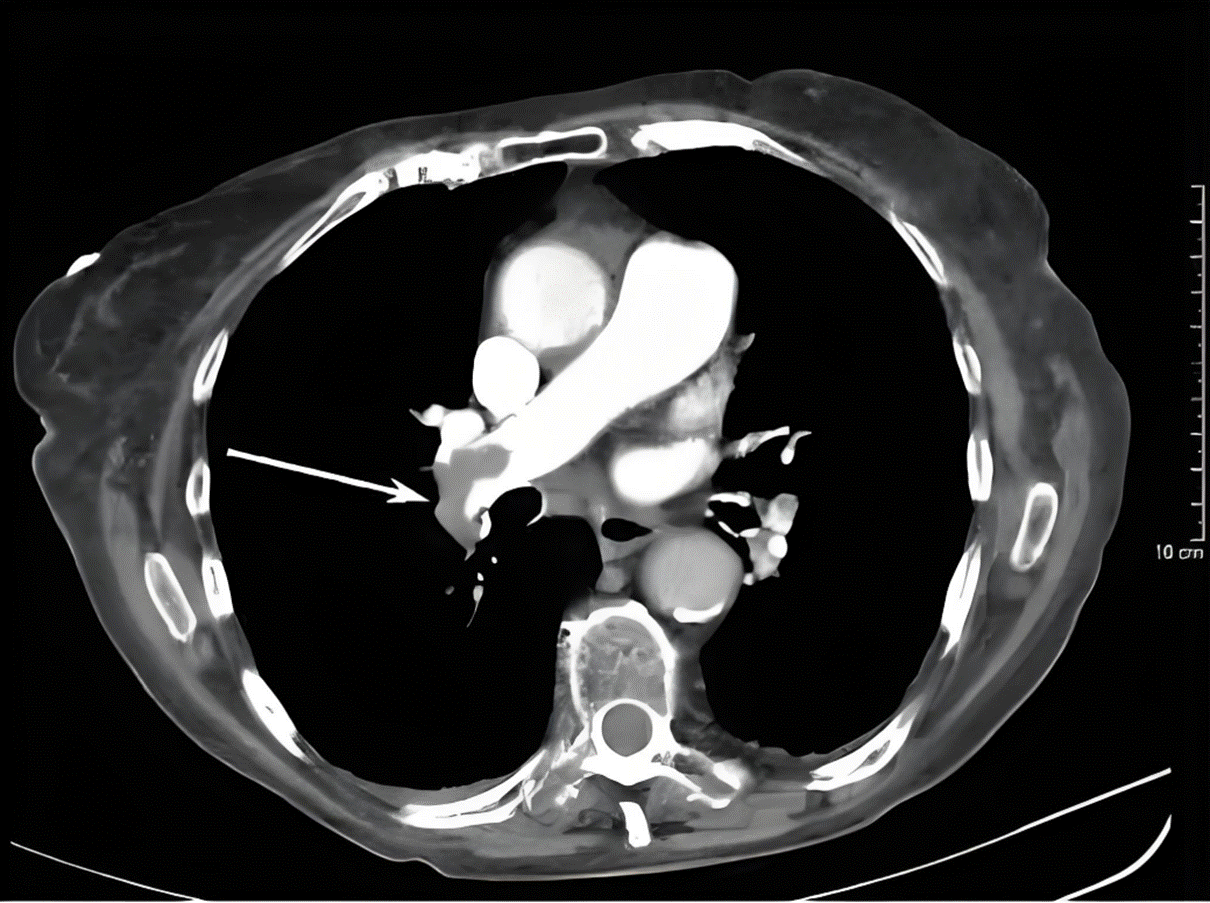
Pulmonary Artery Embolism CT Image (Image source: Internet)
Two . Structure
Superior vena cava + Right heart + Pulmonary artery + Inferior vena cava + Iliac vein + (Iliac bifurcation upward) 2cm Location)
Xi'an Derui Medical has crafted a pulmonary artery interventional vascular model using medical-grade, highly transparent, soft silicone. Its outstanding high-elasticity properties precisely replicate the flexible texture and mechanical characteristics of the pulmonary artery wall—capturing everything from resistance feedback during puncture procedures to subtle tactile changes as instruments are advanced. The model closely mimics the real-life experience of working with human blood vessels. CT Based on imaging data, leveraging advanced 3D The printing process fully replicates the vascular network morphology from the main pulmonary artery down to the segmental arteries, meticulously showcasing intricate anatomical details such as the course of interlobar arteries and the branching patterns of segmental arteries. Additionally, the model features a modular design that allows for rapid replacement of pathological components, enabling flexible simulation of various pulmonary arterial lesion scenarios—including emboli of different shapes, areas of vascular stenosis, and even arteriovenous malformation clusters in the lungs.

Three . Functions and Applications
Function:
The pulmonary artery interventional vascular model plays an indispensable role in clinical diagnosis and treatment as well as medical research. Its primary function lies in preoperative simulation, enabled by its high precision. 3D Printing technology, capable of 1:1 Restoring the complex anatomical structure of the patient's pulmonary artery, including areas with stenosis, malformations, and other lesions, helps doctors plan the surgical approach in advance and anticipate potential challenges during the procedure—such as changes in vessel anatomy or issues with instrument passage—thereby enhancing the overall success rate of the surgery.
In the field of medical education and training, this model serves as an ideal hands-on teaching tool. Medical students and young physicians can repeatedly practice on the model to become familiar with the workflow of pulmonary artery intervention procedures, master critical skills such as guidewire and catheter manipulation, as well as balloon dilation techniques, and gain valuable experience—while minimizing risks associated with inexperience when performing these procedures on real patients.
Additionally, the vascular model can also be used for testing and developing interventional devices. Researchers can simulate various pathological scenarios using the model to evaluate the device’s deliverability, flexibility, and adaptability, enabling them to refine designs promptly and accelerate the development of innovative interventional tools. This, in turn, will provide higher-quality instruments for pulmonary arterial interventions, driving continuous progress in the field.
Applications:
In the field of medical education, vascular models have opened a door “ Immersive learning ” The hospital doors. Medical students no longer have to imagine the procedural steps by staring at anatomical charts—they can now hold catheters in their own hands, feeling firsthand how resistance changes as the guidewire navigates through curved blood vessels on a realistic model. This allows them to practice critical maneuvers like balloon positioning and stent deployment over and over again. “ Visible and tangible ” Their learning approach has significantly accelerated the growth of young doctors.
For the medical device R&D team, vascular models serve as a means to validate innovation. “ Touchstone ” R&D personnel can simulate a variety of complex lesion scenarios to test whether the new catheter has sufficient flexibility to navigate through narrow vessels—and to verify how well stents perform when deployed in tortuous vascular structures. By continuously refining and iterating the models, they ultimately pave the way for safer, more effective interventional devices to reach clinical practice.

Pulmonary artery + Close-up photo of the item below the knee
Keywords:
Other news
Request a quote
*Please keep your phone accessible—we'll reach out to you within 24 hours.









